CPT Code 96130

Jaime Saal, MA, LPC, NCC — Updated April 2026
Billing for psychological testing evaluation services is one of the most underutilized reimbursement opportunities in psychiatric practice. CPT code 96130 covers the clinical interpretation work that happens when you review a comprehensive assessment like MindMetrix with your patient — and it is billable by psychiatrists, PMHNPs, and other qualified healthcare professionals alongside your standard E/M visit code.
This guide covers everything you need to submit a clean 96130 claim: what the code covers, who can bill it, how to document correctly, which modifiers to use, and what to do when a payer pushes back.
What is CPT code 96130?
CPT 96130 covers the first hour of psychological testing evaluation services performed by a physician or other qualified healthcare professional (QHP). The work it reimburses includes:
- Reviewing test results — for example, a MindMetrix report
- Integrating patient data and collateral information
- Interpreting standardized test scores against clinical cutoffs
- Clinical decision-making and differential diagnosis
- Treatment planning based on assessment findings
- Documentation and report writing
- Providing interactive feedback to the patient or family
96130 is a time-based code. The minimum threshold is 31 minutes of total time — this can include both face-to-face time with the patient and non-face-to-face time such as reviewing the report before the appointment and writing documentation afterward. You do not need to spend 31 minutes face-to-face — prep time counts.
Tip: Combined visit prep time and time spent face-to-face with the patient both count toward the 31-minute minimum. If you spend 15 minutes reviewing the MindMetrix report before the visit and 20 minutes discussing results with the patient, you have met the threshold.
Add-on code: 96131
If your evaluation time exceeds one hour, bill 96131 as an add-on code for each additional hour. 96131 cannot be billed alone — it always accompanies 96130.
Related code: 96127
If 96130 is not covered by a particular payer, CPT 96127 is an alternative. It covers brief emotional or behavioral assessments using standardized instruments and does not have the 31-minute minimum. Typical reimbursement is $7–$12 per unit, and most payers cap it at four units per visit. It is a much lower reimbursement than 96130, but it is broadly accepted and can be used as a fallback.
Who can bill 96130?
CPT 96130 can be billed by any physician or qualified healthcare professional. In psychiatric practice, this includes:
- Psychiatrists (MD, DO)
- Psychiatric-Mental Health Nurse Practitioners (PMHNPs)
- Nurse Practitioners (NP) and Physician Assistants (PA) in psychiatric or primary care settings
- Licensed Psychologists and Doctoral-Level Clinicians
- Master's-Level Clinicians — coverage varies significantly by payer contract
Payer note: Master's-level clinicians and licensed counselors are not universally recognized as QHPs for 96130 under CMS guidelines. If you are an LPC, LCSW, or LMFT, verify with each payer before billing this code. Some private payers will reimburse; Medicare generally will not.
Reimbursement rates
Reimbursement rates for 96130 vary by payer, provider type, and contract. As a benchmark:
| Payer type | Typical 96130 reimbursement |
| Medicare (national average, 2025–2026) | $113–$130 per hour |
| Major commercial payers (Aetna, BCBS) | $130–$175 per hour |
| Optum plans | PhD/PsyD only in many markets; verify contract |
| Medicaid | Varies by state; check your state fee schedule |
These amounts are subject to co-pays, co-insurance, and deductibles. To understand your practice's expected reimbursement: review your fee schedules to confirm 96130 is covered, check your contract for authorized provider types, note any carve-outs or rate differences by credential, and confirm state-specific scope of practice limitations.
Billing workflow: how to bill 96130 with an E/M code
For prescribing clinicians — psychiatrists, PMHNPs, and PAs — the standard workflow is to bill 96130 alongside your E/M code for the same visit. Here is how that works:
Step 1: Complete the evaluation (31+ minutes)
Review the MindMetrix report before the appointment (10–15 minutes). Discuss findings with the patient, walk through differential diagnosis steps, and align on a treatment direction (15–25 minutes). Complete documentation and note final clinical impressions (5–10 minutes). Total time easily meets or exceeds the 31-minute threshold.
Step 2: Document using QuickChart
MindMetrix's QuickChart tool automatically generates a structured chart note that populates key findings from the assessment. For 96130, your note needs to include: a summary of psychological findings from the assessment, time-in and time-out for the 96130 portion of the visit, total time spent (prep + face-to-face, minimum 31 minutes), assessment tools reviewed (MindMetrix auto-populates this), and clinical impressions and treatment plan updates.
QuickChart auto-calculates total time and pre-fills the assessment tool list — the sections that require your input are the clinical summary and treatment plan, which you would be writing anyway.
Step 3: Submit the claim with correct codes and modifiers
Bill both 96130 and your E/M code (99202–99215) on the same claim. Use the following modifiers:
| Modifier | When to use |
| Modifier 25 on E/M code | Signals that the E/M is a significant, separately identifiable service from the testing evaluation |
| Modifier 59 on 96130 | Signals that 96130 is a distinct service, not bundled with the E/M |
| Modifier 95 on 96130 | Add after modifier 59 if the session was conducted via telehealth (approved through December 2026) |
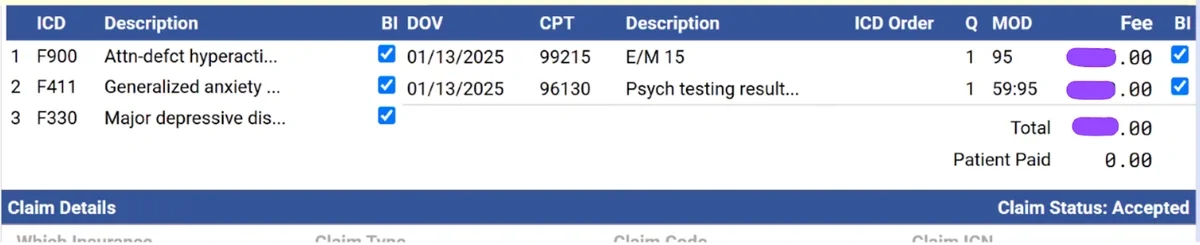
An example of how to bill 96130 along with an E/M telehealth visit:
E/M code selection should be based on medical decision-making, not time — because 96130 is already the time-based code for this visit, and CMS rules prohibit using the same time block to justify two separate time-based codes.
ICD-10 coding for 96130
Mental health ICD-10 codes (F-codes) are required to establish medical necessity for 96130. A critical rule: do not use the same ICD-10 code to justify both your E/M and 96130 on the same claim. Payers may treat the two services as redundant and bundle — or deny — 96130. Use distinct diagnostic codes for each service line, or use the same primary diagnosis but include additional specificity (a more granular subcode or comorbid condition code) on the 96130 line.
Billing 96130 as a non-prescribing clinician
Psychologists, licensed counselors, and other non-prescribers who conduct formal psychological evaluations bill 96130 differently:
- Bill 96130 as a standalone code for the session — do not combine with a therapy code (90832–90838) on the same day
- Document that test results were reviewed, a summary of key findings, any recommendations discussed, and session length (minimum 31 minutes)
- If the session exceeds one hour, add 96131 for each additional hour
Non-prescribers generally do not combine 96130 with E/M codes, since E/M codes are typically used by physicians and mid-level prescribers.
Prior authorization
Prior authorization is typically not required for PPOs billing 96130. Some HMOs may request prior auth. If you encounter unexpected prior auth denials, it is worth appealing — denials often stem from payer staff unfamiliarity with the code rather than a policy exclusion. A brief letter of medical necessity citing the clinical rationale for comprehensive psychological testing frequently resolves these denials.
What if 96130 is not reimbursed?
A small number of practices report that specific payers in their market do not cover 96130. If that applies to you:
- Use 96127 as a fallback: Bill up to four units per visit at $7–$12 each. Lower reimbursement, but widely accepted.
- Bill E/M based on time: If the session is extended specifically because of testing review, you may select the E/M level based on total time rather than medical decision-making complexity.
- Ask about MindMetrix's Dynamic Pricing Program: If none of your payers cover 96130, MindMetrix offers a discounted subscription rate. Contact support@mindmetrix.com with documentation of the denial.
MindMetrix offers a free one-on-one billing consultation for providers who want help submitting their first 96130 claim, understanding modifiers, or navigating a denial. Active subscribers can book directly from the provider dashboard. New providers can request a consult here.
Ready to boost your practice?
Try 3 complimentary assessments on us.