MindMetrix Outcomes Study
Evaluating the Impact of MindMetrix on Psychiatric Symptom Trajectories
April, 2026
There’s a moment at the start of nearly every psychiatric intake where the direction of care quietly takes shape
A few symptoms are shared.
A few screening tools are selected.
A clinical hypothesis begins to form.
But here’s the challenge: What if that initial picture is incomplete?
The Diagnostic Reality We Work Within
Psychiatric conditions rarely present in isolation. They overlap. They evolve. They mask each other.
- Roughly 50% of individuals may live with an undiagnosed mental health condition
- At least 65% of conditions may be misdiagnosed
- Comorbidities are common—and frequently missed
Despite this, most workflows still follow a familiar pattern:
Clinical interview → Select a few screeners → Form a diagnosis
Even with strong clinical judgment, this approach is constrained by time and by what gets surfaced early.
And when we rely on a limited set of tools, we risk narrowing the diagnosis itself.
A More Comprehensive Starting Point
MindMetrix was designed to expand that initial window—systematically.
How It Works
1. Initial Symptom Screen
- Patients review a broad set of psychiatric symptoms and indicate whether each reflects current or past experiences.
- Follow-up questions assess daily impact.
- Symptoms that meet predefined thresholds trigger deeper evaluation.
2. Disorder-Specific Follow-Up (Post-Tests)
- Each triggered pathway deploys up to three validated self-report assessments specific to that condition.
3. Probability-Based Reporting
- Results are synthesized into estimated disorder probabilities using Bayes’ theorem, applying:
- Published sensitivity and specificity values
- Disorder prevalence rates
- Likelihood ratios to refine probability estimates
The output is not just a score—but a structured, probabilistic clinical picture across dozens of potential conditions.
The Study: Does This Actually Change Outcomes?
To evaluate real-world impact, a retrospective longitudinal study examined whether including MindMetrix at intake influences symptom trajectories over time.
Study Design
- Single-site, retrospective EMR analysis
- Adult patients in outpatient psychiatric care (Oct 2023 – June 2024)
- Inclusion: CGI-S ≥ 4 at baseline + at least one prescriber visit
Groups
- +MM (n = 97): Completed MindMetrix at intake
- −MM (n = 50): Standard intake procedures
Baseline Comparability
There were no significant differences at baseline across:
- CGI-S
- PHQ-9
- GAD-2
- ASSET
(all p > .05)
This supports that both groups started from a comparable clinical position.
What Was Measured
Patients completed structured assessments before each visit:
- Depression: PHQ-9
- Anxiety: GAD-2
- ADHD: ASSET
Outcomes included:
- Change from baseline at ~90–120 days
- Symptom correlations and composite psychiatric burden
- Regression models evaluating treatment trajectory over time
What the Data Shows
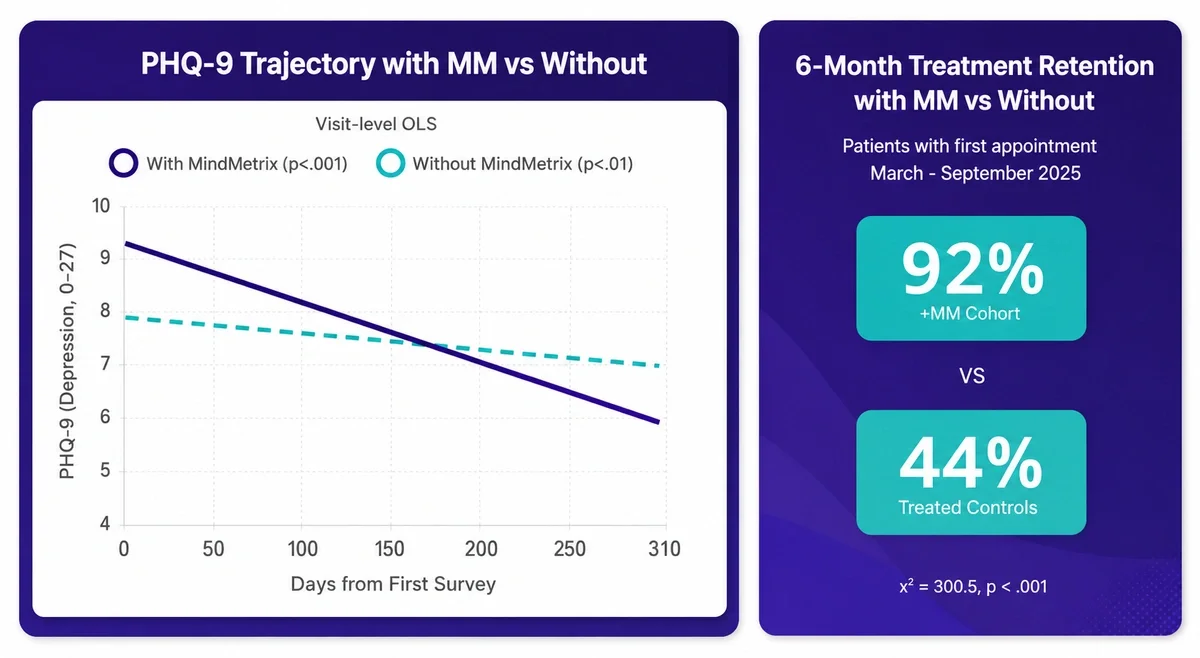
1. Retention in Care Improves
- 64% of patients had a follow-up within 90–120 days
- +MM patients were significantly more likely to remain in treatment:
- 70.8% vs. 46.9%
- OR = 2.75, p = .006
- For patients with high ADHD symptom burden, the difference was even more striking:
- 72.7% vs. 26.7% retained
- OR = 7.33, p = .002
A more comprehensive intake may not just inform care—it may keep patients engaged in it.
2. Symptoms Improve Over Time—But Not Equally
Across all patients: Depression, anxiety, and ADHD symptoms improved with time in treatment.
But, patients who completed MindMetrix improved more, and faster in key domains.
3. Stronger Symptom Reduction in Depression and ADHD
MindMetrix significantly amplified the rate of improvement over time for:
- Depression (PHQ-9): β = −0.857, p = .049
- ADHD (ASSET): β = −0.307, p = .002
No significant effect was observed for anxiety: GAD-2: β = −0.184, p = .158
The impact of a more comprehensive intake may be domain-specific, with the strongest signal in depression and ADHD.
4. Broader Psychiatric Burden Improves More Steeply
A composite symptom factor (derived from PHQ-9, GAD-2, and ASSET) showed:
- Strong intercorrelation across measures (r > .49, p < .005)
- Significant moderation by MindMetrix:
- β = −0.256, p = .001
This was the strongest overall signal in the study.
5. Independent Associations with Improvement
Both MindMetrix completion, and time in treatment were independently associated with greater symptom improvement across all measures (p < .05).
What This Suggests
This is the first empirical study to suggest that incorporating a dynamic, comprehensive assessment like MindMetrix at intake is associated with:
- Greater retention in care
- Faster improvement in depression and ADHD symptoms
- Stronger overall reduction in psychiatric symptom burden
Importantly: Patients improve with treatment regardless, but how they improve may depend on how they start.
A Note on Limitations
As with all real-world evidence:
- Findings are associative, not causal
- Residual confounding is possible
- Results reflect a single-site population
Future research should validate these findings across broader and more diverse settings, ideally through controlled experimental designs.
Final Thought
For years, limited time and incomplete data have been accepted constraints in psychiatric diagnosis. But if a more complete clinical picture at intake is associated with better engagement, faster improvement, and more defined trajectories, then the conversation shifts.
It’s no longer just about whether patients get better. It’s about how much earlier we could have understood what they needed.
Ready to boost your practice?
Try 3 complimentary assessments on us.